Published in TIME magazine
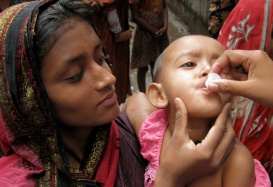
Cholera kills 120,000 people every year, estimates the World Health Organization. Could mass vaccination—now being tested in Bangladesh’s cholera-prone capital—prove a new weapon against an old disease?
By Andrew Marshall
DHAKA — Anita Ashfaqunnesa skips over a ditch oozing with raw sewage, her spotless white shawl trailing behind her like a superhero’s cape, then squeezes between shacks built on an old rubbish dump. Three years ago, she explains, this slum in northern Dhaka didn’t exist. But with hundreds of thousands of rural job-seekers pouring into Bangladesh’s capital every year, it now teems with families, and the water they use for drinking, cooking and bathing comes from pipes that run alongside, and often through, the sewage ditches. That’s why the area’s oldest living resident is not a person, but a disease. “Cholera is a common ordeal here,” says Anita, 33. “People don’t fear it, but they are happy to hear there’s a vaccine coming to prevent it.”
Anita is one of a small army of field workers collecting household data for the biggest oral cholera vaccination program in history. It starts on Feb. 17 and will involve 240,000 residents in Mirpur, the district that reports most of Dhaka’s cholera cases. Two-thirds of them will receive two oral doses of a cheap new Indian-made vaccine. “We think of it as a demonstration project rather than a trial,” says Dr. Stephen Luby, Bangladesh country director for the U.S. Centers for Disease Control (CDC). “We don’t have a big question in our minds over whether this vaccine is going to prevent cholera. What we’re trying to do is illustrate the feasibility of using it as a public health intervention.”
Mass vaccination could be a new weapon against an old disease. In Zimbabwe, where cholera claimed 5,000 lives in 2008 and 2009, a swift vaccination program could have cut the death toll by 40%, calculated the authors of a study published in Jan by PLoS Neglected Tropical Diseases. Such results are avidly followed in Haiti, where cholera has killed about 3,800 people and sickened 189,000 since October. A committee that includes experts from the CDC and the World Health Organization (WHO) recently recommended a small-scale cholera vaccination project. This rankled Haitian health officials, who want millions to be protected against a disease that foreign peacekeepers almost certainly brought with them after last year’s earthquake.
Nobody in Bangladesh disputes the origins of the disease. The Ganges delta, which India and Bangladesh straddle, is cholera’s homeland. Six of the seven pandemics since the 19th century have originated here. Every year, WHO estimates, there are 3-5 million cholera cases and up to 120,000 deaths worldwide. Dhaka’s dilapidated water and sanitation systems provide ideal conditions. Bounded by rivers that are too filthy to purify, the city pumps up nearly all its water from hundreds of deep wells. It is never enough, especially when those pumps need electricity to run, and Bangladesh is plagued by power shortages too. With no positive pressure in the water pipes, sewage and other contaminants easily leak in.
The only thing Dhaka doesn’t lack is people. With 13 million residents and counting, it is a fast-growing megacity in the world’s most densely populated large country. New arrivals squeeze into already overflowing slums, or squat on wasteland with zero infrastructure. “Wherever there is human misery you will find cholera,” says Dr. Mark Pietroni, Medical Director of the International Centre for Diarrhoeal Disease Research, Bangladesh (ICDDR,B) in Dhaka, which is implementing the vaccine project with the Bangladesh government. “It thrives on malnutrition, overcrowding and poor hygiene.”
Cholera outbreaks in Dhaka are as predictable as the seasons. There are two each year: roughly one before and one after the monsoon. Dhaka Hospital at the ICDDR,B treats thousands of cholera patients, who during outbreaks not only crowd its wards and hallways, but spill out into tents in the parking lot, forming what might be the world’s only hospital ward with speed bumps. Left untreated, cholera can kill in hours. But treat it promptly and properly, mainly with oral rehydration salts, and death rates are under 1%. At Dhaka Hospital, even the sickest patients make near-miraculous recoveries; arrive with just one breath, say locals, and you’ll leave alive.
But as Dhaka’s population grows, so does the hospital’s patient load. Every March and April, a thousand new patients a day is standard. “Cholera is a dreaded illness because of its rapid onset, severity and potential to cause outbreaks that easily overwhelm public health systems,” says Dr. Regina Rabinovich, director of Infectious Diseases at the Bill & Melinda Gates Foundation. “That’s why it’s important to invest in the development of new, more effective vaccines.”
Enter Shanchol, a two-dose vaccine produced by Shantha Biotechnics of Hyderabad and developed with funding from (among others) the Gates Foundation, which also gave $16.5 million to the ICDDR,B for the cholera vaccine project. Shanchol is safe and efficacious: a trial in the Indian city of Kolkata involving nearly 70,000 people showed that the drug gave 67% protection for at least 2 years. Just as importantly for mass vaccinations, it is cheap: its two doses cost about $3, or about a tenth the price of its only rival, the Dutch-made drug Dukoral. Shanchol is expected to get WHO approval this year.
Bangladesh’s state-run immunization programs are widely trusted, so persuading a cholera-weary populace to take the vaccine shouldn’t be hard. Some 80,000 adults and children will receive it; another 80,000 will receive the vaccine, plus active encouragement to treat household water and wash their hands with soap. But assuaging those who don’t get it might be trickier. This includes 80,000 people who will unknowingly receive a placebo, forming a control group that helps validate the project’s results. “That’s what we perceive is going to be our biggest problem: not everybody gets it,” says Luby, who was seconded from the CDC to head the ICDDRB’s Program on Infectious Diseases and Vaccine Sciences.
One of the project’s broader aims is to get a better idea of cholera’s mortality rate. “Right now most of the estimates that people throw around are quite speculative,” says Luby. Mortality at the ICDDR,B’s hospital may be less than 1%, but some patients are dead on arrival — negotiating this vast city’s gridlocked streets can use up precious hours — and others expire at home.
Mass vaccination has its critics. Today’s drugs do not offer long-term coverage or protect against every cholera strain. And even a cheap vaccine, in high quantities, is expensive and could divert resources from the only thing proven to eradicate cholera: improved water and sanitation infrastructure. (London suffered centuries of cholera epidemics until the Victorians built sewers.) Improving Dhaka’s infrastructure is vital, agrees Luby, but the task could take decades. The same is true for hundreds of cities in our rapidly urbanizing world, and indeed for disaster zones such as Haiti. While that infrastructure is being built or rebuilt, how do you protect a vulnerable population from cholera? Mass vaccination is one answer. “What we’re trying to do is generate some evidence on what’s feasible and cost-effective,” he says.
Participants in the Mirpur project will be monitored for years. But the vaccine’s impact could be felt as early as March or April, when the more severe of Dhaka’s biannual epidemics strikes. “That’s why we’re aiming to have this community immunized by the time that worst peak comes,” says Luby. Haiti — and the rest of the world — will be watching.
Correction: The people in the control group will not receive a placebo, knowingly or unknowingly. My apologies for the error.









Written by Andrew Marshall
Posted on 15 February 2011